Neglected tropical diseases
“Major obstacle for development”
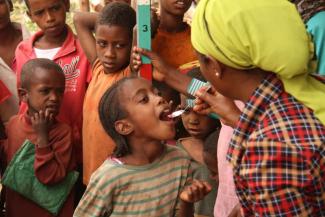
According to the World Health Organization (WHO), 1 to 1.5 billion people suffer from neglected tropical diseases (see D+C/E+Z e-Paper 2018/01, p. 7), and up to half a million people die every year. Nevertheless many of those diseases are still not well known in industrial countries. What are NTDs, and which of them are the most prevalent?
NTDs are a group of 20 diseases. This group is very heterogeneous: some diseases are caused by viruses, others by bacteria, worms or other pathogens. What they have in common is that they are all diseases of neglected and marginalised people. Poor hygiene, weak health systems and a lack of accessible clean water and sanitation make NTDs thrive. The most common ones – the so-called „big five“ – are trachoma and river blindness, which lead to permanent visual impairment or blindness, elephantiasis, which causes severe swelling of parts of the body and is thus very stigmatising, schistosomiasis and soil-transmitted intestinal worms that lead to anaemia, growth inhibition and developmental disabilities. The „big five“ are responsible for about 90 % of the global NTD burden. Other well known examples include leprosy, sleeping sickness, Buruli ulcer and Chagas.
Which of those 20 diseases are chronic?
Most NTDs lead to chronic disabilities that are often very stigmatising, particularly elephantiasis and blindness. Trachoma and river blindness are the leading infectious causes of visual impairment and blindness (see D+C/E+Z e-Paper 2017/06, p. 29). NTDs are also a major poverty trap. They often put an end to a person’s economic productivity. Working-age adults are particularly affected, and that has major implications for their families and communities: a farmer who becomes blind stops being the family’s breadwinner. His children become caretakers and often can’t attend school. Thus, the disease affects the next generation, keeping it trapped in a cycle of NTDs, disability and poverty. Examples for more acute NTDs include dengue fever, rabies and snakebites, recently added to the WHO list.
Mainly people in developing countries suffer from NTDs, particularly women and children. What are the main implications for these – already disadvantaged – groups?
The Sustainable Development Goals (SDGs) pledge to “leave nobody behind”. We all have to understand that we cannot achieve the SDGs if we don’t overcome the massive burden of NTDs. They are a major obstacle for development. The required comprehensive and inclusive approaches include prevention, treatment, rehabilitation and care (continuum of care). For all this it is very important to systematically include affected people with disabilities in our programme work and to promote full inclusion in all aspects of social life. CBM works hard to ensure that these important issues are better understood, make all NTD work inclusive and social settings to become empowering. Stigmatisation and other psycho-social consequences of NTDs, such as depression and anxiety, for example, must also be addressed. Without such comprehensive and inclusive approaches, a sustainable solution is not feasible.
Can the NTDs be treated successfully or – even better – prevented, for instance through immunisation, and ultimately eradicated?
As already mentioned, the group is very heterogeneous. Better immunisation is being developed for certain diseases, dengue fever, for example. For other NTDs, the focus is on reducing or eliminating the risk of transmission. That can be done for instance by mass drug administration (MDA) of the entire population at risk and improved hygiene and sanitation. Apart from better infrastructure, we need to achieve sustained behaviour change. In order to stop the spread of trachoma, for instance, the people at risk must wash faces regularly. They need access to clean water and toilets – and use them. If water must be fetched from far away, which is often the case, the people’s priority is drinking and cooking – not hygiene. That’s why clean water must be accessible close to the home. Toilets reduce the breeding opportunities of certain flies that transmit trachoma and other diseases. Children and women are most affected by active trachoma, and if faces are kept clean, the chance of interrupting transmission is very good. Good and cost-effective eyelid surgery can save people who are threatened by blindness, a long-term impact of trachoma. Certain diseases such as Guinea worm have almost been eradicated; for others the focus is on eliminating them as a public health problem, rendering targeted population programmes unnecessary.
The fifth Progress Report of the London Declaration on NTDs was published in December 2017. It shows impressing achievements in combatting the NTDs. What is the biggest success?
Well, progress towards eliminating trachoma for example has been very encouraging. If we intensify our efforts, we can achieve the WHO Trachoma Alliance goal of providing quality eye lid surgery to those immediately threatened by blindness from trichiasis by 2020. Moreover, the active disease will also be eliminated as a public health problem in many countries by then – but not everywhere. Progress is slowed down particularly in areas of conflict and crises. Overall, we are making promising progress however. The same is true for river blindness. In Latin America, there are only six small transmission zones left. In Africa, which is by far most affected, the number of new cases of blindness has dropped dramatically. That’s a huge success. The drugs required for elimination have to be successfully distributed year after year, to large populations, even during periods of instability and to very remote areas. However, elimination will take longer in conflict areas such as South Sudan, the Central African Republic and parts of the Democratic Republic of the Congo. CBM has been active in Burundi for a long time, and from our experience there we know that a lot can be achieved even in post-conflict countries. Interrupting transmission of elephantiasis is within reach too. As with trachoma, the most important measures are mass drug administration to all communities at risk, improvement of hygiene and sanitation and strengthening health systems particularly at grassroots levels. Now we must also step up support for the many people already affected by chronic disease and disability.
So there are good drugs and successful programmes for many NTDs, but local circumstances can hinder action?
Yes, that’s right for many, but one has to differentiate. There is typically no shortage of drugs for mass drug administration against the “big five”. Pharmaceutical companies have pledged to donate sufficient amounts until elimination has been achieved. The challenge is to reach consistently all people at risk for as long as it takes. Weak infrastructure is another big problem. It enhances the risk of infection, developing chronic disabilities and complicates adequate treatment and care. We have to double our efforts to raise awareness for these diseases and their consequences at all levels, develop local capacities and improve existing diagnostic and treatment tools. Concerning other – less frequent – NTDs, however, we still often lack the appropriate means. Funding and support have to increase and action must be accelerated.
So how is this done and how can affected countries’ health systems be strengthened?
CBM for example works only within national programmes – in close collaboration with affected communities and local health services. Typically, needs are greatest in remote rural areas. Through targeted training, support and awareness activities we help to ensure that drugs and other interventions are reaching those most in need. Improving water, sanitation and hygiene (WASH) and developing local capacity to plan, implement and monitor all activities are other crucial aspects of our work. The cooperation with partners is equally important. We systematically support the health ministries and local partners in countries such as the Central African Republic, the DR Congo and South Sudan, for instance, and collaborate with other international organisations and the WHO, including financial support. Our goal is to share CBM’s vast expertise and experiences with the global NTD community and thus make a lasting positive impact on the lives of affected people and communities.
Where do you currently see the greatest deficits in the international fight against NTDs?
In a twin-track approach, we must reinforce our efforts for prevention and treatment and at the same time, work towards a true continuum of care – ensuring social inclusion and rehabilitation of people with chronic disabilities. To achieve all this money is still short. We already have existing diagnostic and therapeutic tools for the “big five” – but they must be constantly developed further. However, for many other NTDs suitable diagnostics and therapeutics are still lacking. Thus, research and development remain vitally important. Above all, we must raise awareness and the understanding that we cannot achieve the SDGs if we don’t end NTDs. They must be seen exemplary for negligence and underdevelopment.
Martin Kollmann is Senior Advisor on Neglected Tropical Diseases (NTD’s) for Christoffel-Blindenmission (CBM) and co-founder of the German Network against NTDs (DNTDs).
martin.kollmann@cbm.org
Links
German Network against NTDs:
http://www.dntds.de/en/start-en.html
Fifth Progress Report of the London Declaration on NTDs:
http://unitingtocombatntds.org/wp-content/themes/tetloose/app/staticPages/fifthReport/files/fifth_progress_report.pdf










