Editorial
Traditions and modernity
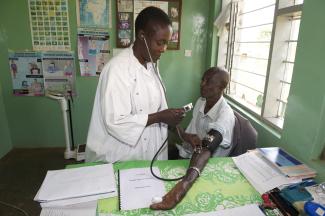
Illness plunges far too many families into poverty when breadwinners can no longer work, or when treatment costs overwhelm household budgets. Limited health, moreover, limits educational opportunities too. That is the case when children with disabilities cannot go to school, when students drop out of university in order to earn money in support of their families, or when adolescent girls stay at home to take care of ailing relatives. As societies age around the world, the latter setting is likely to become more common. Demographic change is a widely neglected global phenomenon.
With reasonable, but not overwhelming success, international donors focussed on three urgent health issues in the past two decades: child mortality, maternal mortality and the infectious diseases HIV/AIDS, malaria and tuberculosis. It was always hoped that helping developing countries to invest in these matters would contribute to strengthening their health-care systems in general. That, however, only happened to a rather limited extent. Typically, the health-care systems in the world’s less advantaged regions do not have enough doctors and nurses. One reason is that many governments cut bud-gets drastically in the 1980s and 1990s, as was demanded by the structural adjustment programmes the International Monetary Fund and the World Bank designed to make highly-indebted countries competitive again. Today, a lasting result is too few and too poorly paid jobs in health care. Doctors and nurses with professional skills tend to find better employment opportunities in richer nations. Good health care has a price.
Health is not something to be left only to doctors and nurses however. Prevention is better than cure. Information and behavioural change are the only way to stem HIV/AIDS and malaria, for instance. Progress in other health issues similarly depends on people assuming responsibility for their own lives. Examples range from drinking only water that is safe for consumption to the early diagnosis of cancer.
Awareness campaigns must have an impact on people’s everyday lives – in villages, at school, at work, in the market square, in churches, mosques and temples. And campaigns must not only convey knowledge; they must also put those they convince in touch with experts who will give advice on personal health issues. If people do not get access to doctors, nurses and other competent persons, no awareness campaign will ever make them change their lives.
Given the dramatic lack of professional staff, prudent policymakers and aid agencies must involve traditional healers in health care in developing countries. Academically trained experts are often uncomfortable with doing so because traditional methods are not necessarily based on science, and some are actually hazardous. Nonetheless, many traditional methods work. And their practitioners have another important advantage: they are in touch with the target groups and enjoy their trust. Health-care systems must not emphasise the clash of modernity with tradition; developing countries need as much cooperation as possible. Over time, moreover, meaningful interaction of both sides will lead to modernising traditional practices bit by bit.