Public Health
“Mental health issues are totally underrated in Africa”
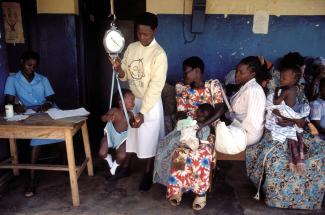
In various African countries, there are different approaches to solving the precarious health situation of poor people. Uganda opted for universal health coverage. Is this a big issue in this nation?
The government favoured universal health coverage, but the health workers were not in for it because the fees paid by patients were abolished, but this used to supplement their pay. The fees also supported medicine purchases, other supplies and facility development. Physicians are lead actors in health development, but often do not appreciate the context they work in. They focus on individual care, not on the community. At the time, people were too poor to pay and many flocked to the health facilities when fees were abolished. The people know what they want, but the health system is letting them down. We need to mobilise the people to participate in our efforts to achieve universal health coverage.
What do you consider essential in health care?
At the minimum, universal health coverage should address women’s and children’s health – that is maternal and child health. The health of mothers and children is crucial for a nation’s growth. At the moment, infant and maternal mortality are too high, compounded by HIV/AIDS, but also because of poverty and lack of adequate care.
Are small-scale saving groups a solution as health insurance for poor people?
Health savings pools can be a solution. These pools have to be re-insured in a national health insurance scheme, though. We want to work with the people through the community pools, and the proposal is before the Ugandan cabinet right now. We have a strategic plan for holistic health financing in the country … hopefully we shall have a harmonised plan for the whole of East Africa.
This sounds like a multi-sectoral approach. Are you joining up with different sectors to lift the Ugandan health-care system to international standard?
A multi-sectoral approach addresses all elements necessary to ensure achievement of health goals for a country. For example, the medical school curriculum could be better in training health personnel. We are linking up with the Ministry of Education which is responsible for this.
There is a joint UN and ILO programme on gender equality in Uganda. Does this influence health issues?
Focussing on gender equality is part of the health agenda. This cross-sectoral approach to gender issues is useful when advancing health reforms.
Internationally, Uganda is seen as positive example for effective high-level response in dealing with HIV/AIDS, significantly slowing down the enormous number of infections that the country had in the 1990s. Why was Uganda able to confront this pandemic efficiently, while other African countries were not?
After the dictatorship of Idi Amin ended, we were left with no institutional structures – traditional or modern – to build on. It was like starting to build afresh. We had strong political commitment at the highest level but we also listened and learned from others.
Could you identify a main health issue in Africa that is possibly underrated in the international discourse?
Mental health issues are totally underrated in Africa. This gets hardly any attention. The focus is on malaria and HIV/AIDS. Lack of resources gets mental disorders relegated to the background. With mental health problems, people consult traditional healers, but this is stigmatised. People suffer from stress due to many reasons, for instance, from the after-effects of war. Today we have more personnel being trained in mental health work in Uganda, so there is hope for the future.
What can policymakers do about this?
The health system needs to be responsive to the actual needs of the people. Health professionals have to understand that health is politics – and politics is about power to allocate resources. Without politics and integrating health policy into the overall macro-policies and plans of governments, achieving people’s health and well-being in developing countries will remain a dream.
Questions by Sheila Mysorekar.
Speciosa Wandira-Kazibwe is a surgeon and was Vice President of the Republic of Uganda. At present, she is an advisor to the President of Uganda on Population and Health, and is reforming the health sector. Furthermore she has been appointed as Special Envoy to the UN Secretary General on HIV/AIDS in Africa.
swandira@health.go.ug