Pandemic
Science-based protection
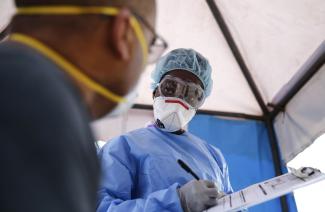
The experience of other continents shows that the strategies to contain the new coronavirus are:
- to detect infected individuals as early as possible by testing,
- then quarantining positive cases and treating the severe ones,
- tracing, tracking and testing people who had been in contact with individuals,
- social distancing in society, whether one is positive or not,
- hygienic practices such as correctly washing hands with soap or effective sanitising agents and
- wearing protective gear, including masks and gloves, if infected or caring for infected patients.
It is obvious, moreover that successful implementation hinges on:
- community participation,
- strong national health-care systems and
- the political commitment and effectiveness of national leadership as well as,
- effective cooperation at national, regional and global levels.
The point is that messaging has to be coherent and convincing. Moreover, people need to see that systems are working to protect them.
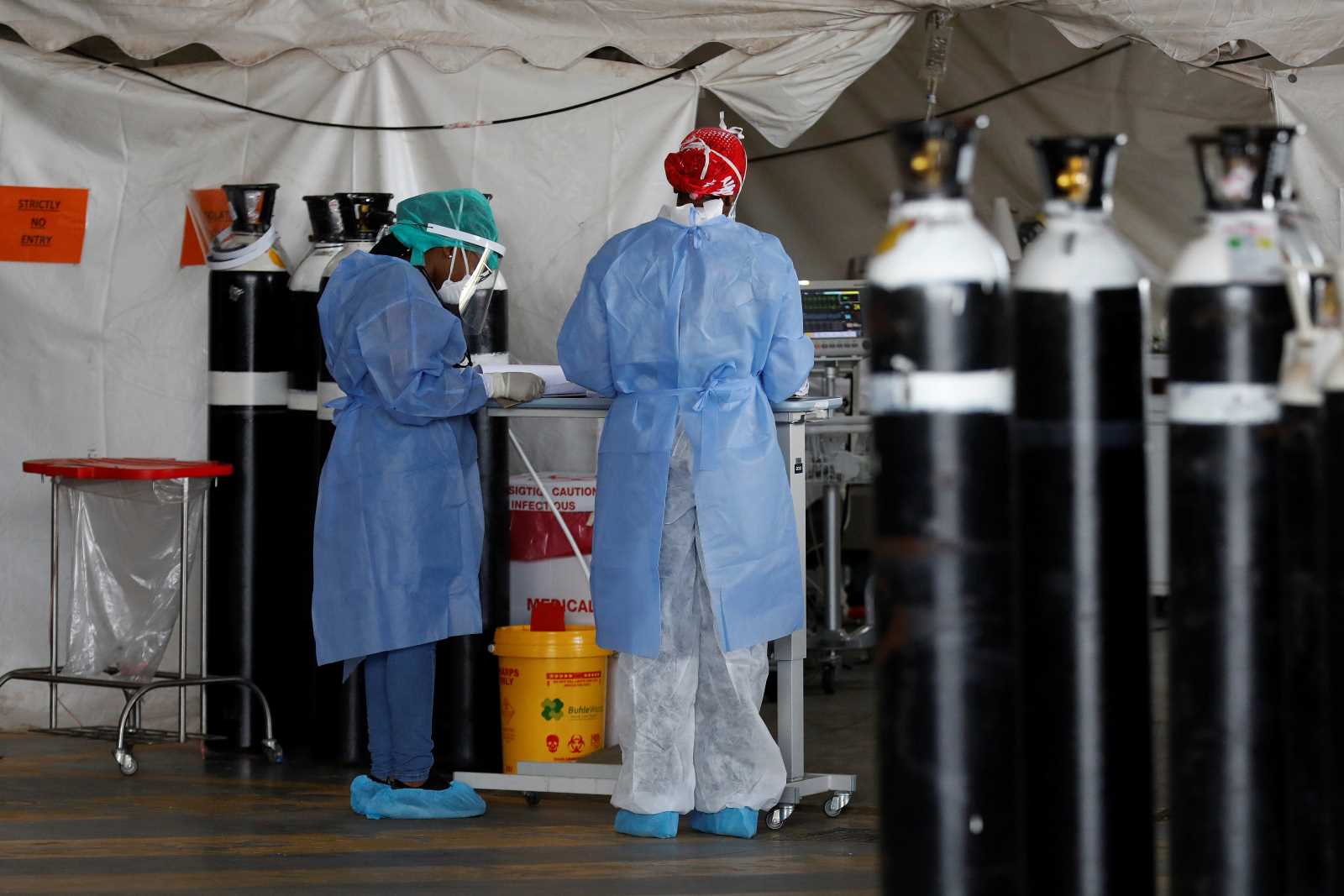
Africa’s health-care systems are generally weak. Typically, they lack sufficient funding and staff. Moreover, institutions in general tend to be weak. Against this background, Covid-19 is likely to prove more devastating than in prosperous nations. On the upside, global, regional and national collaboration has already yielded significant gains. At first, only two African countries had SARS-CoV-2 testing capacities. By 7 April, that number had risen to 47. Testing capacity was continuously improving.
Informal urban settlements cause concern nonetheless. They are characterised by overcrowding, endemicity of tuberculosis (TB) and HIV, as well as limited access to water and basic services. All of this will likely fuel the spread of Covid-19. Some 200 million to 300 million people live in such conditions. Their neighbourhoods are too densely populated for stringent social distancing. Harsh measures to enforce a lockdown, however, cannot work in places where people depend on daily wages for their livelihoods. Ultimately, evidence-based and context-specific measures will ultimately determine success. Otherwise, the pandemic is likely to take a massive toll on human life.
African governments have closed borders, declared states of disaster or emergency, imposed curfews or even imposed a complete lockdown. They are investing in health-care systems. Their public awareness campaigns rely on mainstream media as well as social media. Hotline numbers allow people to contact relevant government offices.
Most likely, additional response measures will be developed and implemented. Mobile phones are common, and Africa has come up with valuable digital innovations in recent years. Creative solutions are needed now, especially in health care.
Globally and in Africa, the economic consequences of the COVID-19 pandemic are already obvious. Many businesses are at risk of collapsing and this is already resulting in the loss of jobs. Supply chains of essential goods and services are threatened. So far, it is hard to see how African governments can limit the economic damage. They do not have the financial resources to pass rescue packages of the kind seen in the EU or the USA.
The pandemic will amplify food insecurity in Africa, already a major concern as millions of people suffer from starvation and under- and malnutrition. The negative impacts on the immune systems of the people concerned make them more susceptible to infections. No doubt, African countries now require global solidarity.
The pandemic also creates opportunities in the longer run. Authorities will better understand the connection between health and economy, and that should catalyse the strengthening of health-care systems. Strong regional cooperation established now can create a framework for better coordination in the future.
Benjamin M. Kagina is a senior research officer and vaccinologist with the Vaccines for Africa Initiative (VACFA) at the University of Cape Town’s School of Public Health and Family Medicine.
benjamin.kagina@uct.ac.za