Health
How to contain superbugs
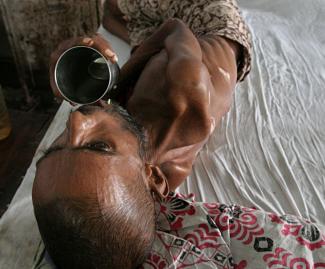
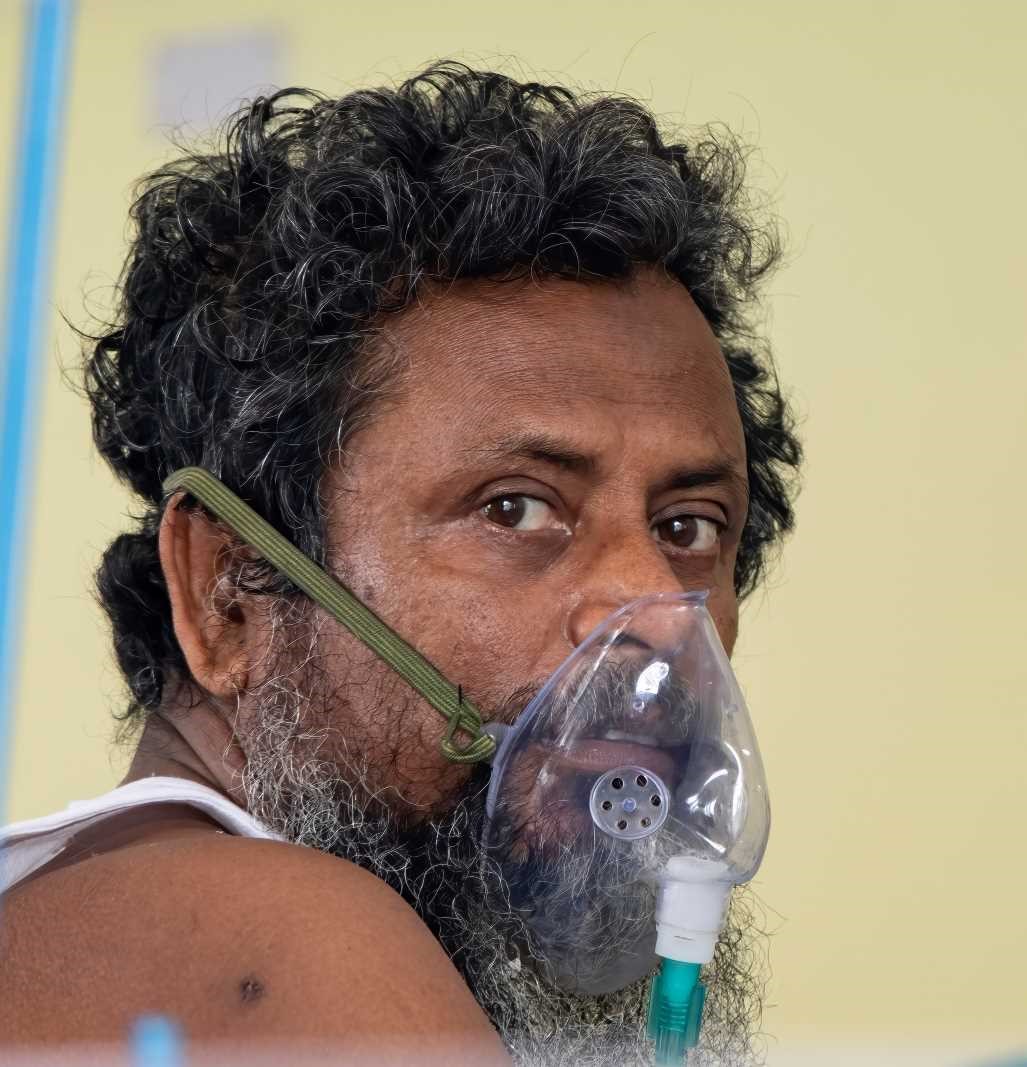
The World Health Organization (WHO) has recently classified antimicrobial resistance as one of the 10 greatest threats to global health in 2019. There are indeed ever more reports of how antimicrobial resistance is making some infections almost impossible to treat. Developing countries are hit hardest.
Antimicrobial resistance is not restricted to one particular pathogen or disease. This fact makes it harder for policymakers and the general public to understand the urgency of the issue and act accordingly. Drug-resistant “superbugs” are therefore not high on the international agenda. Unfortunately, momentum was neither sustained in 2016, after the UN General Assembly passed a declaration on the matter, nor in 2015, after the World Health Assembly adopted a global action plan.
Antimicrobial resistance is a natural evolutionary process which makes a commonly used antibiotic ineffective. Bacteria mutate and become immune to agents that previously killed them. The overuse and misuse of antimicrobial substances in health care, animal husbandry and agriculture accelerates this natural trend.
Inadequate use of antibiotics is driven by many things, including over-aggressive marketing by pharma corporations and inappropriate prescription guidelines. In developing countries, antibiotics are all too often applied to handle the consequences of insufficient water and sanitation infrastructure. Heavy reliance on antimicrobial agents in agriculture compounds the problems. Even antibiotics that are important for human health or even last-resource medication are used on farms.
The international community needs joint action to stop such malpractice in health care and in agriculture. Special interests will try to defend their profits, but the top priority must certainly be the sustainability of health care. It is a global public good.
The depressing truth is that we are running out of treatment options for ever more strains of illnesses such as gonorrhea, malaria and tuberculosis. Measures to tackle the superbugs are complex and require multi-sectoral action. Developing countries cannot rise to the challenges on their own.
No doubt, developing countries must strengthen their health systems, ensure access to clean water and improve infrastructure as well as public services in general. These are development challenges they must rise to. More is needed, however, and essential pharmaceutical research and development (R&D) is extremely expensive. It is needed to:
- make new treatment options available,
- improve diagnostic and laboratory infrastructure and
- monitor the spread of superbugs.
R&D exceeds the funding capacities of developing countries. This is evident in the plain fact that superbug infections kill fewer patients in developing countries than the unavailability and unaffordability of standard antibiotics. Poverty actually is one of the factors that accelerate the spread of antimicrobial resistance. The reason is that cash-strapped patients often stop using antibiotics too early. Satisfied that the symptoms are gone, they stop spending money on the drug and visiting the doctor. What they do not know is that their infection has not yet been cured and the surviving bacteria are more likely to mutate into drug-resistant strains.
Tuberculosis is a case in point. It remains the number-one killer infection. Multidrug-resistant strains make it ever harder to treat. New treatments (bedaquiline and delmanid) have come to the market, but they are out of reach for patients – and governments – in countries with high disease burdens.
Action at the global level needs to be geared to mobilising resources, tools and finance. Developing countries must be enabled to respond to the health challenges they face. Since deadly diseases do not respect national borders, antimicrobial resistance is a global problem. Solving it will require international cooperation. Unless we consider underlying structural causes and implement changes internationally, medical progress will be jeopardised – not only in developing countries.
Mirza Alas is a researcher at the South Centre, the Geneva-based think tank that is owned by developing countries.
alas@southcentre.int