Rural health care
Medicines and supplies are difficult to find in rural Malawi
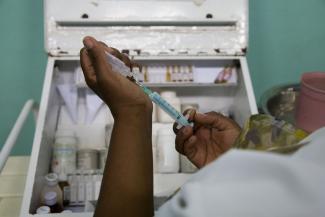
For the rural poor in Malawi, medicines and medical care are in short supply. A good example is found in Naisi, a rural area outside of the town of Zomba in southern Malawi. The Naisi region’s villages are within the jurisdiction of the Traditional Authority of Malemia, which has a population of about 18,000. Its people are poor, mainly subsistence farmers.
The region is supposed to be served by the Naisi Health Centre, a rural clinic run by the government. The underfunded clinic relies on international aid for medications. Medicines and medical supplies are in fact being sent – but sometimes they do not reach the intended recipients. In some cases this is because of confusion and excessive burdens at local clinics.
“We often see vehicles loaded with items we believe to be the medicine and other essentials meant to aid our community, but when we need medication we are told it is unavailable,” says Chikondi Leveni (real name withheld), a farmer and domestic worker in the village of Mtewa.
“Conditions at the Naisi Health Centre are poor,” she adds. “It‘s almost impossible to get a correct diagnosis, and it‘s hard to get medication even for something as common as malaria. I was once critically ill with malaria. After I waited nearly an hour at the centre, a health-care worker only gave me Paracetamol, which slightly reduces fever. I was told to buy more Paracetamol at the pharmacy, which I cannot afford.”
In Chisupuli, a village near Mtewa, Aisa Kazembe (real name withheld) had similar experiences. An elderly woman, Kazembe suffers from hypertension. “The health facility barely has medication available for conditions like mine,” she says. “The last time I went to the health centre my blood pressure was high and I needed urgent medical attention. However, the medical worker told me I might be overstating. I wasn‘t given any diagnosis or medication. I had to go to a private clinic, which is costly. It was a horrible experience.” Her experience was not unique, she adds: “We are often left desperate and we don’t know whom to turn to. If nothing is done, the lives of many of us will be at risk.”
Asked to respond, a senior clinician at the Naisi Health Centre told a reporter to first obtain a letter from the District Head Office (DHO) authorising the clinic to comment publicly. An official at the DHO produced a letter but refused to sign it, saying health workers are only allowed to speak with reporters who are recognised by the Ministry of Health.
However, a disease surveillance assistant in Naisi who requested anonymity says the health centre is burdened by incompetence and lack of accountability. He adds that the DHO and other government bodies should supervise such clinics more closely to improve the service they deliver to patients. “The way local patients are treated by health workers at most local clinics is quite degrading and unhealthy,” he says. “The patients are vulnerable people in need of help, and they deserve better.”
Above all, he says, once medicines arrive in the region the authorities should make certain that they reach the intended beneficiaries. “If people aren‘t getting their medications, then something is certainly not being handled right,” he says. “Such issues need to be dealt with urgently.“
Sumeya Issa is a freelance journalist in Malawi.
sumieissa@gmail.com