Medical services
Science-based clinic or witch doctor?
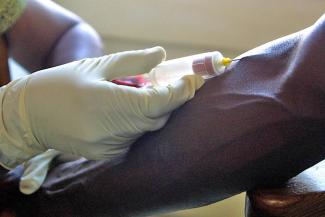
Georgette Viatonou is a mid-career nurse at the Ogan’la medical centre in uptown Porto-Novo, Benin’s capital. Before she receives me in her air-conditioned, but cramped office, she throws a brief glance at her moped to make sure it is padlocked. Thefts of motorcycles are recurrent here. In her office, there are piles of drugs stashed on a shelf and in a big plastic container. She apologises for the lack of space, but she does not complain about the harsh conditions she works in.
Before she turns up for work every morning at 7:30 a. m. some 40 patients line up to see her. They live with HIV/AIDS or suffer from other infectious diseases, including tuberculosis (TB) and malaria. “The patients with HIV/AIDS and tuberculosis often look stressed out, you can read the fright in their eyes,” Georgette tells me. “My day usually starts with group counselling,” she explains. “People living with HIV/AIDS often need to be reassured, they want to hear from me that their condition is not terminal, that they will make it back to a somewhat normal life.” Anti-retroviral drugs make that possible, but they have to be administered diligently. Medication is supplied in sufficient and predictable quantity by the government and the Global Fund to Fight AIDS, Tuberculosis and Malaria.
Nonetheless, there are bottlenecks. Some desperately poor people who are HIV positive cannot afford to pay for clinical and toxicological tests, which cost the equivalent of about € 20. The tests are absolutely indispensable to administer the medicine properly. The centre is required to make patients pay the tests. Despite many difficulties, Georgette does have a nice story to tell. One day, a young woman in her early twenties came for help. She was HIV positive, completely emaciated and almost at a terminal stage. “To be perfectly honest, I saw death in her eyes,” Georgette says. But a few weeks later, the young woman came back, totally rejuvenated. “The antiretroviral drugs that I gave her worked,” Georgette explains. “I gave her a big hug, and encouraged her to continue the treatment.” In the meantime, the young woman gave birth to a healthy baby girl, and Ogan’la’s mid-wives helped her deliver safely.
Ogan’la is a typical public outpatient clinic in Benin. It covers barely 600 square metres in area, its walls are decrepit and in urgent need of fresh paint. The black and red colour of the roofs’ corrugated iron bears testimony to the corrosive effect of the tropical sun and precipitations. There are only a few chairs and benches, so some patients must wait for their turn standing upright.
Ogan’la has an HIV/AIDS treatment unit, a small maternity clinic, a free health-care unit and a small laboratory. It also has an immunisation unit against yellow fever, meningitis and other tropical diseases. About 44 medical personnel are permanently employed here. Ogan’la depends on funding from the Ministry of Health. Most services are not free, but subsidised.
Private providers
In contrast, the Complexe Medico-Chirurgical Santé Pour Tous is a private practitioner’s office in downtown Porto-Novo. It is run by Dr. Moussa Tidjani-Serpos, an old, physically disabled medical practitioner. Here too, decrepit walls and rickety furniture date back to another era, but the fees are much higher. Many patients come here. Tidjani-Serpos, who is assisted by only two nurses, tries to do many things at once: receive patients, listen to them carefully, administer emergency care, help pregnant women deliver their babies, carry out clinical tests, record data on his workstation, issue prescriptions and so forth.
Tidjani-Serpos says that, depending on their financial resources, people in Benin choose between visiting modern clinics and turning to traditional healers. Even witch doctors have a strong presence, especially in rural areas. Their business thrives thanks to poverty, illiteracy and ignorance. Belief in mystical forces is common. Witch doctors often lump fetish practices with herb power – and sometimes it works!
Tidjani-Serpos says that, while some diseases found in Benin are hard to heal, some kinds of common diarrhoea or flu are not hard to heal. Moreover, traditional healers know how to treat broken bones. Some infections are quite serious, however: “Chickenpox threatens the lives of many children.”
Illias Sylla Doucoure is a traditional healer who relies on medicinal herbs. His office, which also serves as his living room, is located in Zongo, a populous neighbourhood of Cotonou, Benin’s commercial centre. The dirt road leading to Doucoure’s house is full of stagnant water and decomposing rubbish. Visitors must hold their breath because of the stench. Yet it is incredible how much the herb doctor knows about both modern and traditional medicine. He first begins with statistics, stating plausibly that some 10,000 traditional herbalists provide health care in Benin, and 80 % of the people trust their services. He says efficient traditional malaria drugs cost three times less than drugs sold in science-based pharmacies.
Doucoure believes that, apart from the low costs, herbalists’ 24-hours-a-day, seven-days-a-week availability is a comparative advantage. Another strong point, according to Doucoure, is that herbalists address illnesses that relate to the physical world as well as those that relate to meta-physics, psychology and spirits. In his view, some illnesses are rooted in an ancestor’s wrongdoing. “Once you find out about the nature of that offense,” he explains, “you make sacrifices to appease the spirits, and the ailment goes away”.
Doucoure does not oppose scientific medicine in principle, however. He appreciates the annual CFA 30 billion (about € 46 million) that the Global Fund gives Benin. Accordingly, drug supply is reliable. “Benin rarely runs out of stock,” he says, “and I salute the efficiency of our national drugs supply and distribution system.” He also praises the health ministry which now plans to officially recognise traditional medicines after testing, certification, approval and patenting procedures.
Doucoure is saddened, however, by the mushrooming of unapproved private health-care centres in Porto-Novo and Cotonou. According to Dorothee Kinde-Gazard, the health minister, some 2,200 illegal health-care centres have been identified across the nation and closed down. They had never undergone any medical inspection. Making matters worse, their staff did not have the required qualifications, and their equipment was often sub-standard. The sad truth, however, is that there simply are not enough health professionals in Benin, as many have left the country. Work is easier and better paid in Europe and North America.
The government wants parliament to pass a new law in order to bring order to Benin’s chaotic health-care business. A huge challenge is stemming the sales of imported counterfeit drugs, which are sub-standard and hazardous. Patients’ demand is huge in Benin, and for scores of people, science-based, up-to-date medicine remains out of reach.
Karim Okanla is a lecturer in media studies, communication and international organisations at Houdegbe North American University in Cotonou, Benin.
karimokanla@yahoo.com