Health and safety
“I am passionate about humanitarian work”
You have worked in many crisis regions. Does your work involve personal risks?
Oh yes. I joined MSF in 1996 when there was civil war in Sierra Leone. We often experienced crossfire. I was directly attacked several times and had to hide myself not to get killed. My posting as head of mission in Kabul, Afghanistan, in 2015 was also very challenging. And in the Somali region of Ethiopia, I have been confronted with many attempts of kidnapping along the Somalia border. Sometimes, we were kept for hours at checkpoints without knowing why and what was going to happen. The situation in 2013 in South Sudan after the political crisis between President Salva Kiir and Vice President Riek Machar was very concerning too. So the risks are part of the job.
How do you cope with these experiences?
Well, when you are in the situation, you don’t realise the danger immediately. Only when you are out, you do. Sometimes you have to get away to survive. At MSF, we have different mechanisms in place. First there is training. We learn what to do in case of different emergency situations – such as gun fire, kidnapping et cetera. That is crucial because if you do the wrong thing, it can be very dangerous. After any critical incident, we withdraw affected staff. Our social units take care of them, offer counselling and try to find out what they need. There are always several options. Some people get evacuated after a critical incident, some get treated at the headquarters or somewhere else, others just need some time to rest. Anyway, whoever doesn’t feel confident anymore is free to go back home.
As a matter of principle, humanitarian agencies do not take sides, but do their best to help suffering persons. Do you always manage to be seen as neutral?
The humanitarian landscape is becoming more and more blurry. Today, even perpetrators pretend to be humanitarian helpers. Access to crisis regions is granted at different fronts, for instance through the government or local authorities, by people with arms or ordinary local people. In some cases, local authorities are party to a conflict, and they might present you as a partner. So we try to clearly communicate our mandate. That is sometimes very difficult, especially in times of social media. People tend to see you as biased. Previously, it was easy, but it is getting ever more difficult.
What do you do to keep people aware of your neutrality?
It’s a continuous process of communication with all parties to the conflict, all persons involved in our work, all stakeholders. We tell them why we are here, what we are doing and why we are doing it. Medical action is based on medical needs. It is not politically controlled, and we don’t want to be linked to any group that is party to the conflict. Everybody must know: MSF is neutral and independent. We really do our best to stick to that mandate.
We have talked about political dimensions and violence – but how about health risks for humanitarian workers? How big are they?
We are always confronted with challenges of that kind. There is a constant risk you might be exposed to deadly diseases like Ebola or Lassa fever. Malaria is endemic in many places, so people do get exposed to it. Some people end up going home due to infections. However, at MSF we try to do as much as we can for prevention and to know the health situation in places we work. But sometimes it’s difficult. People go from one place to the other, and an infectious disease may manifest itself in a new location where it hasn’t been before. So we are constantly monitoring such scenarios.
It seems like your staff must be prepared to take a whole range of risks. Do you know of any people who quit working for MSF because of bad experiences?
Of course I do. For example, in 2013, two female MSF workers were kidnapped in Kenya and held in Somalia for 21 months. When they were released, it was too much for them. We often have that kind of discussion: can we go on or not? I myself had a friend who was shot dead in Somalia. So for me it would be very difficult to work there again. I’m not saying I wouldn’t go there at all. But it’s obviously not my first choice. Not because of the danger. But because my friend’s killing will always come back to me, like a reflection.
What is you personal motivation to keep working in dangerous environments to help other people?
That’s a good question. When I go home after being exposed to a critical situation my first reaction is: “I have to stop!” But then I realise that my input is really positive, that I am saving lives. I joined MSF when I was very young. I passed through many bad situations. But you know, we are providing life-saving intervention on the spot, and I am part of this. That’s a big reward. People come to me and say “thank you for being here, thank you for helping”. That gives me motivation. I am passionate about the humanitarian part of my work.
After postings for MSF in many countries, you now head the mission in Nigeria. What are you doing there?
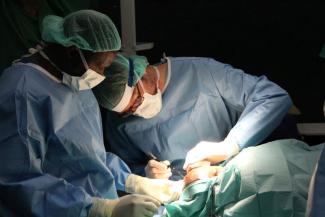
In Nigeria, we have been active in the north-western part of the country for the past ten years. For instance, we respond to outbreaks of diseases such as measles, meningitis or cholera. In Sokoto State, we support a public hospital for Noma patients. Noma is an infection that leads to severe disfigurement of the face. We bring in expatriates to do surgery four times a year, and we support the Ministry of Health to raise awareness for the disease. In a general hospital in Zafara State we have a paediatric ward where we provide medical care for children up to the age of 12. Another project concerns lead poisoning which occurs due to very rudimentary local mining methods in the States of Zamfara and Niger. We are also active in central Nigeria, where land conflicts frequently cause displacement, and we are supporting five camps for internally displaced persons (IDPs) in Benue State. Because of the conflict in Cameroon, Nigeria gets refugees from there too. And then there is irregular migration from Nigeria to Europe. Most of these people come from Edo State, and we are now looking into the reasons for them to leave and what their needs are. MSF has different sections, by the way, and our mission in Nigeria reports to the Operational Centre Amsterdam. It provides emergency medical assistance to people in danger in more than 60 countries.
That sounds like a big range of projects. How big is the team?
The number of staff varies. Currently our team has about 300 national employees and 35 expatriates.
Do the local people appreciate your intervention?
We have to distinguish between the different parties that are concerned. The direct beneficiaries really appreciate what we do. The needs are so acute, and we are more or less the only ones in certain areas that have the capacities to tackle the people’s health problems. The authorities also generally appreciate our work. But each time there are changes in our projects, we have to inform the stakeholders. Communication is crucial, but it’s not always easy to do, so there might be some deficits.
Does terrorism by Boko Haram affect your projects in northern Nigeria?
In the northwest, terrorism is not an issue. But in 2016 and 2017 we were working in the northeastern part of the country, and there has been a lot of terrorism activity that affected the population. There is no frontline. But the local people have been put into a sort of enclave where they are protected by the military. That is the only area where aid workers are allowed to work. Outside, you always have to be aware of landmines or road attacks. It can be very serious. We withdrew from there – but not because of the dangers involved but because many actors are present in that region. So we decided to hand our projects over to other organisations such as International Medical Corps and Oxfam.
Philip Aruna is head of mission for Doctors without Borders (Médecins sans Frontières – MSF) in Nigeria.
http://www.msf.org/en/where-we-work/nigeria