Our view
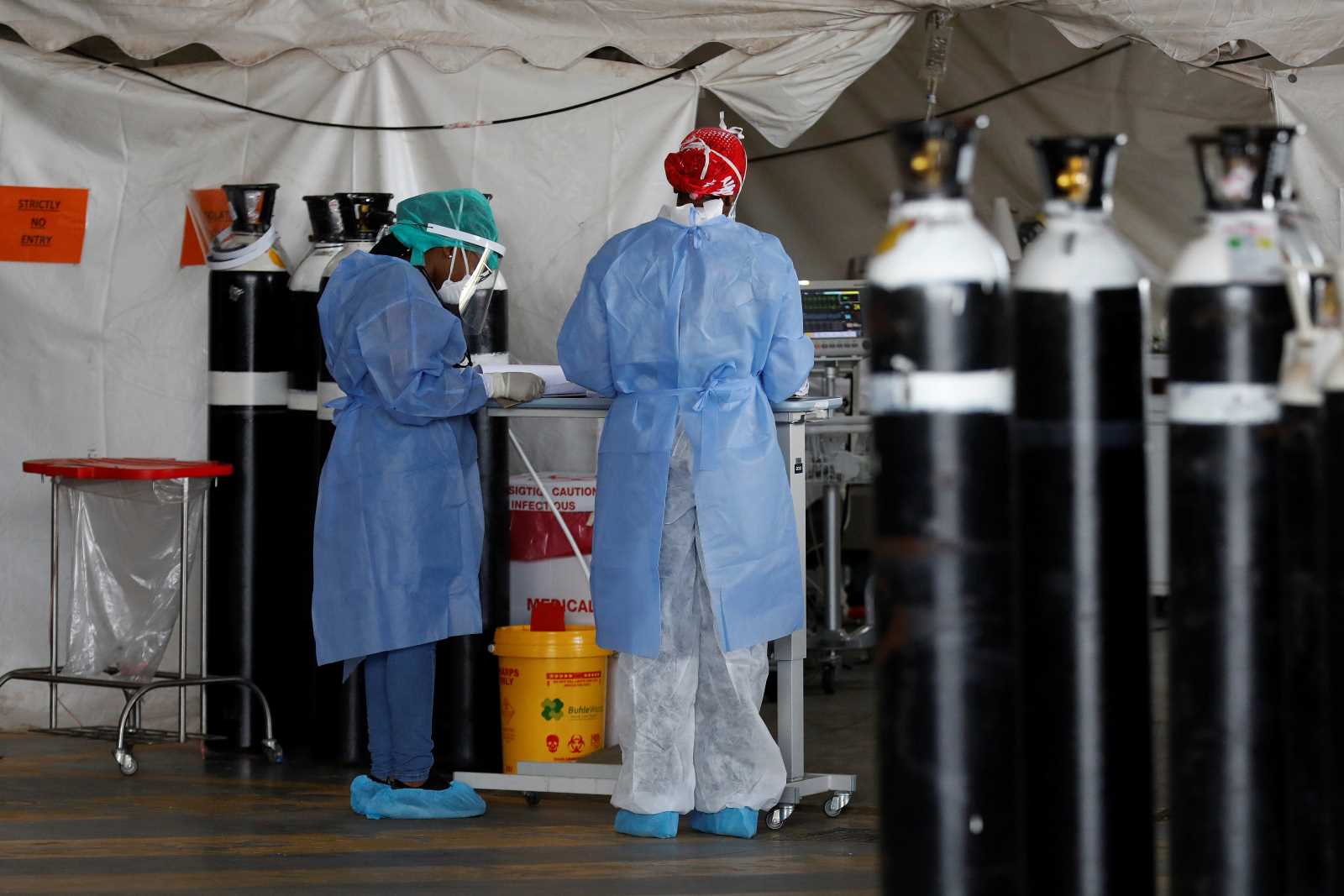
In the health sector, government action is indispensable
The most important reasons are:
- Healthy people often shy away from buying health insurance, so when they do fall seriously ill, treatment far exceeds their purchasing power.
- On the other hand, sick people will often pay any price for anything they believe may help. Entire families drop into poverty this way.
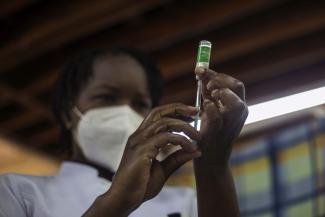
- Health-care measures often produce “public goods” which benefit more persons than the individual buyer. Vaccinations are a good example. A jab not only protects the person concerned from infection, it also prevents that person from spreading the disease.
As Covid-19 is a global pandemic, Covid-19 vaccines are global public goods. Humanity has a shared interest in vaccinating as many people as possible everywhere. If the coronavirus keeps spreading in some places, new mutants will keep emerging there – and those variants will sooner or later haunt places where vaccination campaigns have supposedly provided safety.
In early 2020, policymakers around the world emphasised the public-good dimension. In recent months, we have nonetheless witnessed vaccine nationalism. Vaccination campaigns took off fast in Britain and the USA – where governments claimed all vaccines produced in their countries for domestic use.
In this context, the debate on patents for innovative pharmaceuticals has re-erupted. To some extent, it is a distraction. Scaling up vaccine production requires much more than the legal permission. Important constraints include technological know-how and ingredient supply. Intellectual property (IP), moreover, does not necessarily limit production. Oxford University has set a good example in its deal with AstraZeneca, insisting on low vaccine prices and generous licensing.
One good example, of course, does not solve the underlying problem. Global IP rules are indeed inconclusive. In principle, every country is allowed to grant compulsory licenses for the production of any drug its health sector depends on should patent holders keep that drug unaffordably expensive. In practice, however, dominant powers have ensured that this right is not made use of systematically, so many patients in developing countries do not get life-saving medication they need. This must change. After all, the UN motto for the Sustainable Development Goals (SDGs) is “leave no one behind”.
Patents make sense when goods are freely traded on markets, helping inventors to maximise profits thanks to a monopoly. Anyone who wants the product, must pay – and those who do not pay, are excluded from the benefits.
In health care, this approach is extremely brutal. In contrast to most consumer goods, there are no substitutes of essential pharmaceuticals. Moreover, vaccination campaigns promote the common good, so governments typically lead them. Indeed, the Covid-19 vaccines we have today, have largely come about thanks to state action in the form of generous research subsidies and guaranteed mass demand. Profit maximisation is not the only or even the main driver of health care – and the goal must be to treat every patient and ensure the provision of public goods.
In this regard, the decisions of the G7 summit in Cornwall fell utterly short. The International Monetary Fund (IMF) had urged the seven leading western powers to adopt and fund a proposal for accelerating health care fast. It was in line with demands raised by an independent panel which had evaluated the global pandemic response on behalf of the World Health Organisation. The sad truth is that the G7 did nor rise to this urgent global challenge even though the sums involved were modest.
Hans Dembowski is editor in chief of D+C Development and Cooperation / E+Z Entwicklung und Zusammenarbeit.
euz.editor@dandc.eu
Update: The final paragraph was added on 30 June.