Chronic disease
Silent epidemic
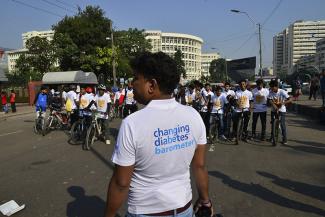
Not long ago, diabetes was considered a disease of prosperous nations that only affected the Global North. Nowadays, millions of people around the world suffer from this chronic condition. According to estimates by the International Diabetes Federation (IDF), almost 80 % of adult diabetics now live in low- and middle-income countries.
It’s true that awareness of the growing impact of non-communicable diseases has increased in development policy circles. That progress is due in part to greater efforts by the World Health Organization (WHO) and the United Nations. While the need for treatment keeps growing, many policymakers still focus on infectious diseases in particular, as a few key facts show:
- It is estimated that about half of all diabetes cases are never medically diagnosed. This is why experts speak of a “silent epidemic”.
- Diabetes affects every world region. Experts estimate that in the future the largest percentage increase will occur in sub-Saharan Africa.
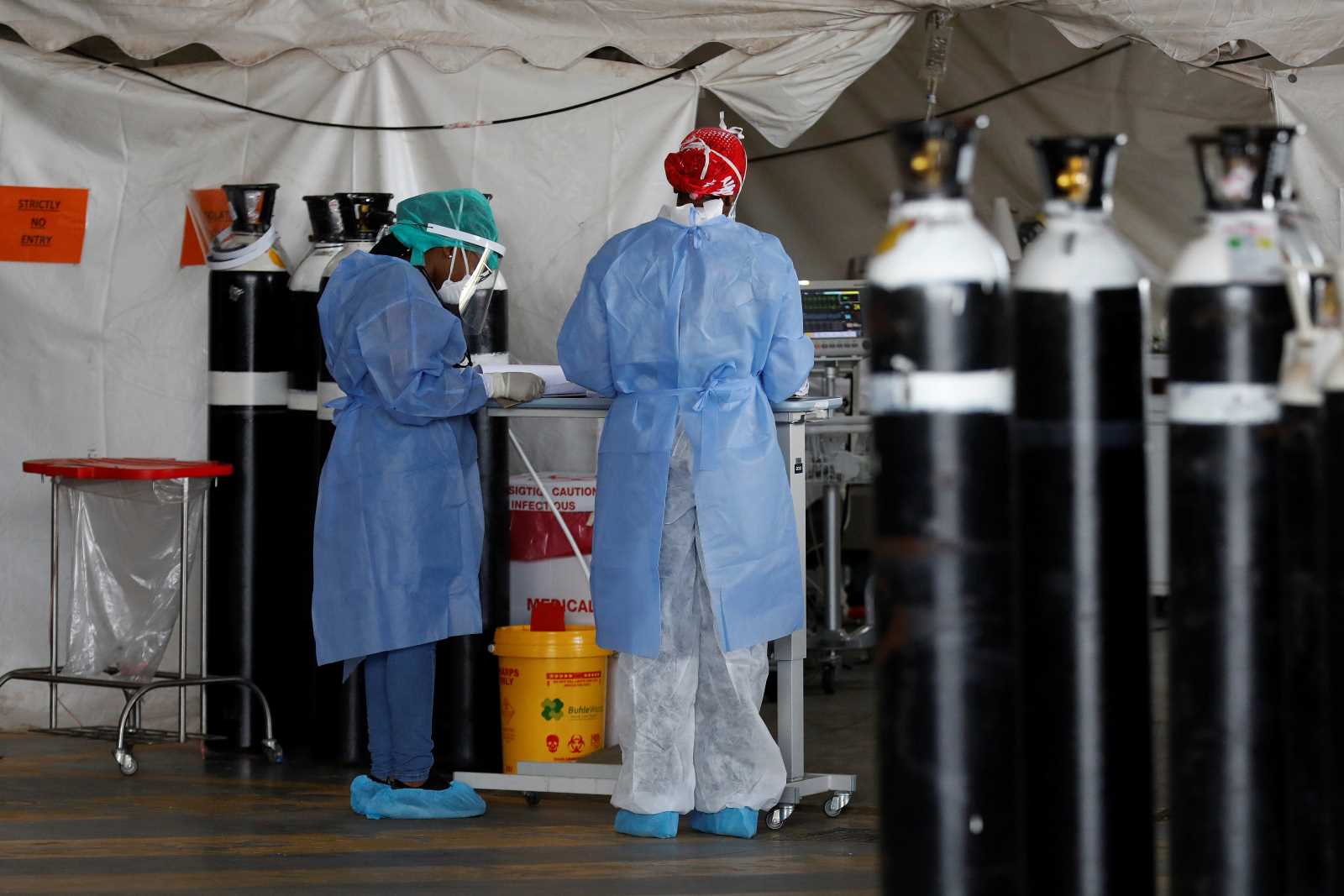
- Millions of patients do not get the insulin they need. They lack access not only by logistical hurdles, but above all by the high price. Just three large pharma corporations control over 95 % of the global insulin market.
If the situation remains unchanged, an enormous gap will emerge between the glaring need for sustainable anti-diabetes measures and the limited scope of funding as well as implementation.
More than a medical problem
Diabetes is a complex disease, which, left untreated, can lead to serious and sometimes even deadly complications (see box next page). Poor patients particularly struggle to get the help that they need. The disease typically exacerbates their economic plight, for example when an adult loses his or her eyesight to diabetes and can no longer work.
The fight against diabetes requires a multifaceted, coherent approach. What is needed is not only better diagnosis, treatment and counselling of patients, but above all prevention. However, prevention should not just address individual behaviour and risk factors. Changing unhealthy lifestyles, for instance through legal regulations, is the most promising way to reduce diabetes rates. Development projects should take this into account in fields like economics, nutrition, education and urban planning.
A few Latin American countries are setting good examples. They have undertaken meaningful efforts to combat the dramatic increase in obesity in children and young people. Along with Ecuador and Mexico, Chile has come up with measures that have attracted attention. The country introduced mandatory warning labels, for instance on products that are high in salt or sugar, as well as stricter requirements regarding the advertisement and sale of such products. Furthermore, Chile’s government raises a considerable tax on drinks with high levels of sugar, but has lowered the tax on products with low levels of sugar. Since the 1970s, some cities in Colombia have also occasionally made more public spaces available to citizens for athletic excercising, for example by temporarily blocking major roads for that purpose.
Greater transparency, greater accountability
Generally speaking, civil-society actors should try to make politicians, donors, foundations and ministries aware of the issue and reach out to the affected groups of people. Both government agencies and private-sector companies must be held accountable for practices that harm health. In poorer communities, for example, food corporations like Nestlé purposefully build networks to sell their products to customers door-to-door. What’s more, tobacco companies are increasingly forcing their way into new markets in countries of the Global South. According to the WHO, almost 80 % of all smokers worldwide now live in low- or middle-income countries. Smoking increases the diabetes risk. Moreover, it contributes to vascular problems, which are typical, dangerous complications of this chronic disease. Civil society organisations must raise awareness for these problems and demand political action.
Fighting for accountability can be quite challenging. That is true even in Germany, where the Federal Ministry of Food and Agriculture is still opposing sensible proposals for a sugar tax.
Civil-society initiatives cannot tackle the causes of diabetes on their own. What is needed is government action – and that may include government protection. In Colombia, for instance, some activists who have challenged powerful economic groups face threats and have reason to fear for their lives.
In both public-sector health care and civil-society health projects, diabetes should be viewed as a cross-cutting issue. It affects everything, from mother-child health to the fight against infectious diseases. Existing structures could be used. In Malawi, for example, measures to treat TB served as a model for similar action to tackle diabetes. Local health-care staff can play important roles. Nurses already lead programmes on mother-child health. They should be trained to spread information about diabetes.
Changes need to be made with regard to research and access to medication as well. Many diagnostic methods and medications were designed to meet the needs of wealthy countries. Not all of them suit developing and newly industrialising countries. For instance, keeping insulin at the appropriate storage temperature can be a serious challenge. Furthermore, high drug prices have led to inadequate supplies worldwide – sometimes resulting in death.
Governments and international organisations must take action to end the multinationals’ insulin monopoly. Insulin prices must drop. On World Diabetes Day 2019 (14 December), the WHO finally published plans to push for that.
The plain truth is that the current market situation should never have arisen in the first place. Insulin is actually a historical example of just how important public research is. This drug was originally developed at the University of Toronto, which decided to forgo patent revenues to ensure all patients got access. In the case of this life-saving drug, price problems are only a very recent phenomenon, which proves that multinational corporations are enjoying excessive market power.
Link
Online course by BUKO Pharma-Kampagne on diabetes in the Global South (2018) (only in German):
http://www.bukopharma-online-lernbox.de/diabetes/
Max Klein is a political scientist and a member of the BUKO Pharma-Kampagne team.
info@bukopharma.de